Immediate Breast Reconstruction
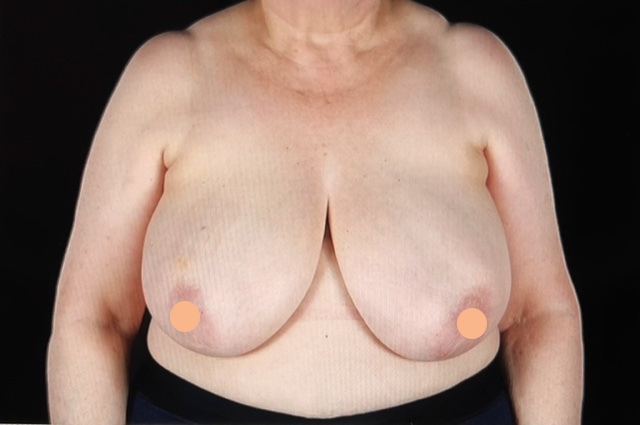
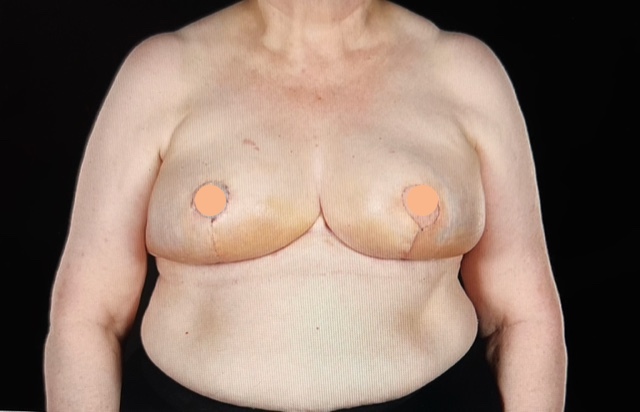
Breast reconstruction will be discussed with all patients who are recommended to have a mastectomy for the treatment of their breast cancer. Not all options and strategies are appropriate for all patients but a bespoke discussion and plan will be discussed. For some patients though immediate breast reconstruction may not be recommended as it may compromise their breast cancer treatment. In that situation breast reconstruction at a delayed point may then be discussed. The key aims of breast reconstruction are volume replacement and symmetry. For many patients, undertaking breast reconstruction will create a different shape and volume to the other non-affected breast. Hence a discussion on symmetry surgery such as an uplift or breast reduction will be undertaken if necessary.
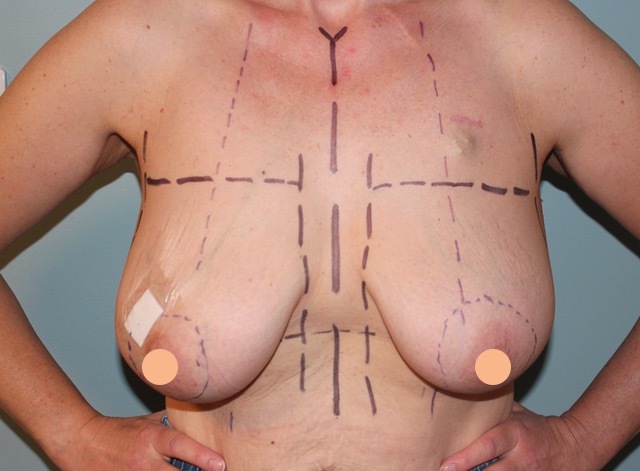
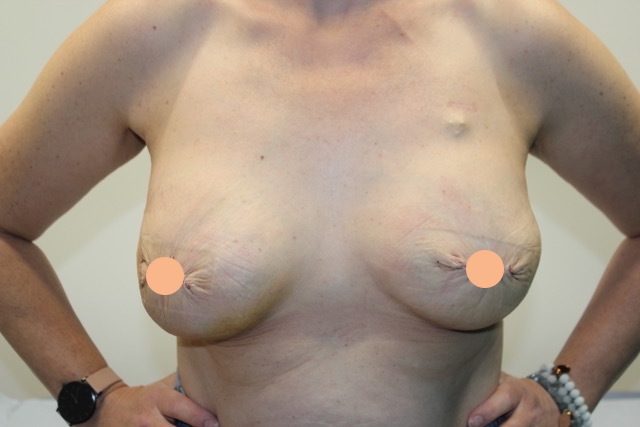
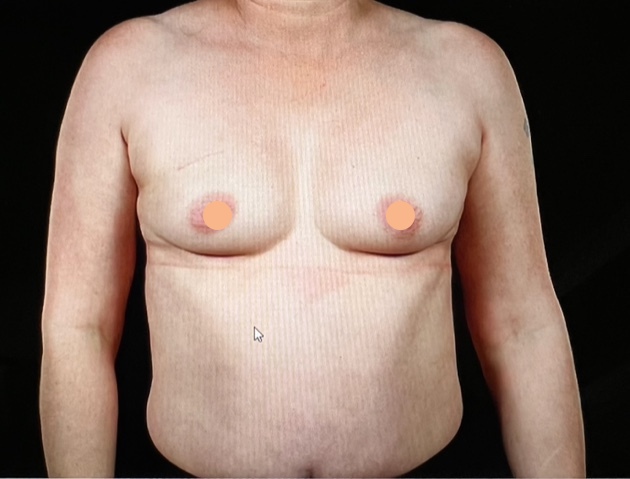
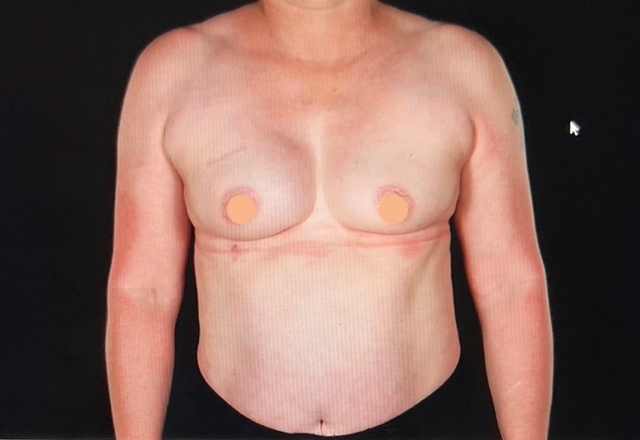
The key options for breast reconstruction are either the use of an implant or your own tissue (usually the back flap or the tummy flap). Each of these options have differences in the length of surgery, length of recovery and risks. There will also be certain occasions where some of these options may not be suitable at the time of mastectomy due to the need for cancer treatments after surgery. In this instance a 2 stage reconstruction can be undertaken where a temporary reconstruction is first done and then after further cancer treatments the final reconstruction can then be completed.